Information for patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
Your The leaflet contains information on what you should be doing before your surgical date and from leaving hospital until your first physiotherapy appointment.
Before Your Surgery
Getting Ready
- You and your doctor will decide if surgery is the best choice.
- You will go to a check‑up appointment called Pre-Assessment to make sure you are well enough for surgery.
- The surgery team will explain the operation and ask you to sign a form to say you understand in a separate consent appointment.
- You will be sent a date for your surgery from the booking office. This will be after your pre – assessment appointment however you may know your surgery date before or after the consent appointment.
Getting Strong First
- Doing exercises before surgery helps your knee get better faster.
- The physiotherapist will show you what to do.
- Think about time off work and who can help you at home.
- You will get a cryocuff, a cold wrap to help with swelling and pain. This will be given to you following surgery and before you leave the hospital.
Why may I need surgery?
- Your knee may feel wobbly or may “give way.”
- If exercises alone do not help, surgery can make your knee more stable.
Two Types of Surgery
Repair – fixing your own ligament if it is not fully torn.
AND
Reconstruction – replacing the ligament if its fully torn.
What happens during surgery?
- You will be asleep for the operation.
- The surgeon looks inside your knee with a tiny camera.
- They remove the torn ligament (if needed).
- They put in a new one called a graft.
Where does the new ligament come from?
- A piece of your own tendon (from your knee, thigh, or hamstring).
- A piece from a donor (someone who has died and chosen to help others).
- A man‑made (synthetic) ligament.
The surgeon will discuss with you; the best one for you.
How do they fix it?
- They make small holes in your bones.
- They put the new ligament through the holes.
- They hold it in place with screws or buttons.
After surgery
- The surgeon checks your knee is strong and moves well.
- You wake up in a recovery room.
- You go home the same day when you feel okay.
What are the possible risks after ACL surgery?
Most people do well, but sometimes these things happen.
- Infection – about 1 in 200 people get an infection.
- Blood clot – about 1 in 250 people get a blood clot in the leg or lung.
- Nerve problems ( numbness) – very rare, about 1 in 150 have a nerve problem.
- Stiff or sore knee – about 3 in 100 people have a stiff knee that needs extra help.
- New ligament does not work (needs another surgery) – about 3 in 100 people need another operation within 5 years.
Exercises from discharge until first physiotherapy appointment
The aim of these exercises is to:
- Restore the movement of your knee; to be able to bend and straighten your knee fully.
- Improve the strength in the leg muscles after the operation.
Complete the exercises several times a day; little and often is best in the days after surgery.
It is normal to feel some aching, stretching or discomfort during the exercises, and for up to 30 minutes after stopping.
If there is big increase in pain you should reduce the frequency, and number of repetitions and talk to the physiotherapist at your first appointment.
Inner Range Quads
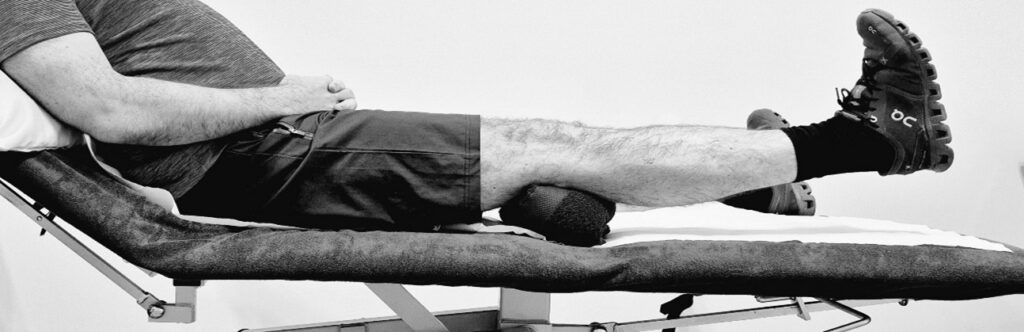
Sit with your legs up on your bed/settee. Place a pillow, rolled up towel or wedge under your operated knee. Bend your ankle, straighten the knee and push it down against the towel/pillow. Then lift your leg 1 cm off the towel. Hold for 10 to 15 seconds. Return to starting position. Repeat 10 to 15 times.
Assisted Chair Knee bends

Sit on a chair with your feet on the floor. Bend your knee as much as possible. Cross your legs at the ankle with the non-operated leg on top and push your operated leg back to bend the knee more. Hold for 5 to 10 seconds. Repeat 10 to 15 times.
Heel Raise

Stand. Push up onto your toes. Hold for 5 to 10 seconds. Lower down. When this becomes easy, try this exercise whilst standing only on your operated leg. Repeat 10 to 20 times.
Sit to Stand to Sit

Sitting with your arms crossed. Stand up from and sit down slowly onto a chair (this can be made easier and more difficult by changing the height of the chair). Repeat 10 times. 2 to 3 sets.
Passive Knee Extension

When sitting place your operated leg out in front of you. If you are on a bed or sofa then place cushions or a rolled-up towel under your heel so the back of the knee is not supported. This can also be achieved with the foot on a foot stool or chair and the knee unsupported.
Place your hand above the knee cap and apply pressure to the front of your knee pushing the leg straight. Hold for 20 seconds and repeat 4 times every few hours during the day.
Extension Holds
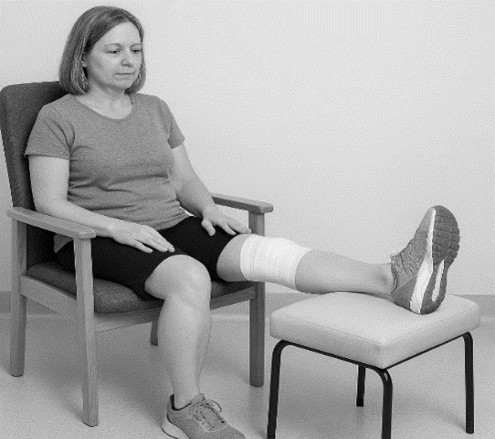
On an evening you should aim to sit in this position and hold it for a sustained time of about 60 minutes. You can do this whilst icing the knee, watching TV or before you go to bed. If the knee aches holding it for this length of time, then you may bend it a few times every now and then to release the tension, then go back into this position until the hour is completed.
Information for discharge following surgery
You will be given crutches following your surgery and you will be taught how to use them before being discharged home. You should use the crutches until advised by your physiotherapist, they are essential to control the load through your knee and to develop a normal walking pattern quicker after your surgery.
Pain relief after your surgery is required to help you perform the exercises and restore normal walking. Your knee will be sore following the operation and you will likely be given a short course of painkillers. If the painkillers you have been given are not sufficient, please contact your GP to discuss alternative options.
Following your surgery, it is recommended you apply the P.E.A.C.E and L.O.V.E. advice.
PEACE (right after surgery)
P – Protect
Keep your knee safe.
Use your crutches. Do not walk too much or do anything that makes your knee hurt more.
This gives your knee time to calm down.
E – Elevate
Lift your leg up so your heel is higher than your hip. This helps swelling go down. You can lie on the sofa or bed and put pillows under your leg.
A – Avoid Anti‑Inflammatories (like ibuprofen)
Some medicines that reduce swelling can slow down healing of the ligament. Only take the pain medicine your doctor or physiotherapist says is safe.
C – Compress
Use your cryocuff or a stretchy bandage around your knee. This helps stop swelling and gives your knee gentle support.
E – Educate
Learn what is normal and what is not. Your physiotherapist will teach you how much to move, how much to rest, and what exercises to do. Understanding your recovery helps you feel more confident and in control.
LOVE (as you start to heal)
L – Load
Start using your leg a little more when it feels safe. This means slowly putting more weight on it and doing gentle exercises. Moving helps your knee get stronger.
O – Optimism
A positive mindset helps your body heal. Feeling calm, hopeful, and supported makes recovery easier. Worry and fear can make pain feel worse.
V – Vascularisation
Do light activities that make your blood flow, like gentle walking or using a bike with no resistance. Good blood flow helps your knee heal faster.
E – Exercise
Do the exercises your physiotherapist gives you. These help your knee bend, straighten, and get strong again. Exercise is one of the most important parts of your recovery.
When can I return to work?
You should have been given a fit note by the hospital if required after your surgery. The length of this fit note will depend on a few factors including the work you perform. For any concerns, please speak with the surgical day unit team prior to discharge or your own GP.
When can I drive again?
Your surgeon will advise you when you can start driving again but it will be a minimum of six weeks or whenever you can comfortably put weight through your operated leg. Your physiotherapist will be able to provide guidance on when you may be able to start considering short journeys but it is your responsibility to ensure you are always in control of the vehicle and can perform an emergency stop effectively.
Contact Information
University Hospital of North Tees
Orthopaedic Outpatients
Telephone: 01642 383838
Email: [email protected]
Monday to Friday, 9:00 am to 4:00 pm
Physiotherapy Admins
Telephone: 01429 522471
Website: https://www.nth.nhs.uk/services/trauma-orthopaedics/lower-limb/
Monday to Friday, 9:00 am to 4:00 pm
If you have any immediate concerns outside of these hours, please contact 111 or attend your local Urgent Care Centre/Minor Injuries Unit.
Further Information
Below are some links to further information and useful videos showing some of the above procedures being performed.
- BMJ Practice (2021)Anterior Cruciate Ligament Injury https://bestpractice.bmj.com/patient-leaflets/en-gb/html/1290088617511/Anterior%20cruciate%20ligament%20injury
- British Journal of Sports Medicine (2020), The ACL Injury Journey – A guide for Patients.
https://blogs.bmj.com/bjsm/2020/12/22/the-acl-injury-journey/
- Arthrex (2024), ACL Reconstruction Using the Synergy Vision™ Imaging System.
https://www.arthrex.com/knee/acl-btb-graft-fixation
- Arthrex (2018), Atraumatic Hamstring Tendon Harvester
https://www.arthrex.com/knee/acl-hamstring-graft-harvest-and-preparation
- Arthrex (2021) GraftLink® ACL Reconstruction Using TightRope® ll Implant for the Internal/Brace™ Technique
https://www.arthrex.com/knee/allinside-acl-reconstruction-flipcutter
References
- Iriuchishima, Takanori, and Bunsei Goto. “Systematic review of surgical technique and tunnel target points and placement in anatomical single-bundle ACL reconstruction.” The Journal of Knee Surgery 34.14 (2021): 1531-1538.
- Murray, MM. Optimizing outcomes of ACL surgery—Is autograft reconstruction the only reasonable option? J Orthop Res. 2021; 39: 1843- 1850. https://doi.org/10.1002/jor.25128
- NHS: Knee ligament surgery, https://www.nhs.uk/conditions/knee-ligament-surgery/, [accessed 21/12/22].
- Pautasso, Andrea, et al. “All-inside technique in ACL reconstruction: mid-term clinical outcomes and comparison with AM technique (Hamstrings and BpTB grafts).” European Journal of Orthopaedic Surgery & Traumatology 31 (2021): 465-472.
- Wittig, Ulrike, et al. “Application and surgical technique of ACL reconstruction using worldwide registry datasets: what can we extract?.” Journal of Functional Morphology and Kinesiology 7.1 (2022): 2.
- BMJ Best Practice, Patient leaflets, Anterior cruciate ligament injury, Patient information from BMJ, Anterior cruciate ligament injury- Patient Leaflet | BMJ Best Practice, [14/12/22].
Patient Experience Team (PET)
North Tees and Hartlepool NHS Foundation Trust would like your feedback. If you would like to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Team who will help you to do this.
This service is based at the University Hospital of North Tees but also covers the University Hospital of Hartlepool, our community hospitals and community health services.
North Tees and Hartlepool NHS Foundation Trust
Telephone: 01642 624719
Freephone: 0800 092 0084
Email: [email protected]
Monday to Friday, 9:30 am to 4:00 pm
Out of Hours
If you wish to speak to a senior member of Trust staff, please contact the hospital switchboard (numbers below).
| University Hospital of North Tees | University Hospital of Hartlepool |
| Hardwick Road Stockton-On-Tees TS19 8PE Telephone: 01642 617617 | Holdforth Road Hartlepool TS24 9AH Telephone: 01642 617617 |
Leaflet reference: PI023 – Version 01
Date for Review: 16/03/2029