What is the Medial Patellofemoral Ligament?
MPFL stands for Medial Patellofemoral Ligament. It is a strong band from the inside of your kneecap over to the inside of the thigh bone. It helps keep your kneecap in the right place. If your kneecap moves out of place (called a dislocation), this ligament can tear.
Why do I need surgery?
If your kneecap keeps moving out of place or feels wobbly, your doctor may suggest fixing or replacing the ligament. This helps your knee feel stable again. It might help with pain, the main reason for the surgery is to improve stability of the kneecap.
How does it tear?
It often tears when your kneecap moves out of place. This can happen during sport or after a fall. Sometimes the kneecap goes back by itself, but the ligament may still be damaged.
What happens in the operation?
- You will go to hospital for the day.
- You will have medicine to make you sleep (anaesthetic).
- The doctor will make small cuts on your knee.
- If the ligament can be fixed, the doctor will sew it back to the bone.
- If it is badly damaged, the doctor will use a piece of tendon from your leg to make a new ligament.
- The cuts will be closed with stitches or clips.
After the operation
- Your knee will feel sore and swollen.
- You will go home the same day or stay one night.
- You will need exercises to make your knee strong and bend again.
- Sometimes, you cannot bend your knee much at first. Your doctor and physiotherapist will tell you what is safe.
- You may need physiotherapy for up to 6 month.
- Do not play sports until your doctor says it is safe.
- Do not drive until you can do an emergency stop and use the car pedals safely.
Benefits of the surgery
- Your kneecap should stop moving out of place.
- Your knee should feel more stable and you can increase your level of activity.
Risks and how often they can happen
- Problems with anaesthetic – Very rare, but can include heart attack or stroke. More likely if you have heart or lung problems.
- Infection – Less than 1 in 100 people (less than 1%).
- Blood clot – About 1 in 1,000 people.
- Nerve damage – Small nerves near the skin can be cut, causing numbness or tingling. Bigger nerves are rarely injured (about 1 in 300 surgeries).
- Knee pain – Some people have pain behind the kneecap or when kneeling.
- Knee stiffness or weakness – Can happen long term in some people.
- Graft failure – The new ligament might fail (small chance).
- Bone fracture during surgery – About 1 in 100 people.
If the first operation is unsuccessful, further surgery may be recommended. But further operations are often more difficult and do not usually have the same long-term success rate as a first ligament repair.
Other choices
You can try exercises and special knee supports instead of surgery. This works best if your kneecap is showing a small amount of extra movement or occurs on certain activities.
If you do nothing your knee might get worse and cause pain or arthritis in the future.
The future
- Most people make a good recovery after a MPFL surgery and are able to return to normal activities without their knee caps dislocating.
- It is unlikely however that your knee will ever feel as it was before the original injury.
Exercises from Discharge until first Physiotherapy appointment
The aim of these exercises is to:
- Restore the movement of your knee; to be able to bend and straighten your knee fully.
- Improve the strength in your operated leg muscles.
Please note: sometimes after surgery, you will be asked to reduce how far you bend your knee on the advice of the surgeon to protect the new ligament.
You will be told before surgery if there is likely to be some limits placed on you bending your knee and for how long. You will be reminded of any restriction before going home from the hospital.
If this is the case you will be informed of the range you are allowed to move and should continue these exercises as far as you are able to within the allowed range of movement.
Complete the exercises several times a day; little and often is best in the days after surgery.
It is normal to feel some aching, stretching or discomfort during the exercises, and for up to 30 minutes after stopping.
If there is big increase in pain you should reduce the frequency, and number of repetitions and talk to the physiotherapist at your first appointment.
Inner Range Quads
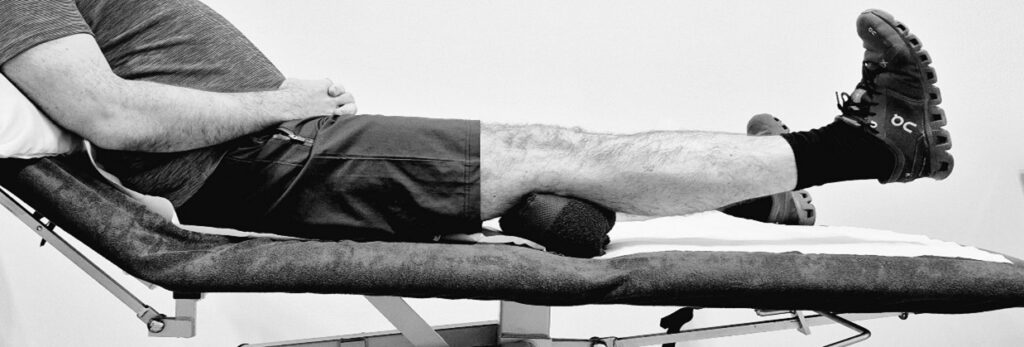
Sit with your legs up on your bed/settee. Place a pillow, rolled up towel or wedge under your operated knee. Bend your ankle, straighten the knee and push it down against the towel/pillow. Then lift your leg 1 cm off the towel. Hold for 10 to 15 seconds. Return to starting position. Repeat 10 to 15 times.
Assisted Chair Knee Bends

Sit on a chair with your feet on the floor. Bend your knee as much as possible. Cross your legs at the ankle with the non-operated leg on top and push your operated leg back to bend the knee more. Hold for 5 to 10 seconds. Repeat 10 to 15 times.
Heel Raise

Stand. Push up onto your toes. Hold for 5 to 10 seconds. Lower down. When this becomes easy, try this exercise whilst standing only on your operated leg. Repeat 10 to 20 times.
Sit and Stand to Sit

Sitting with your arms crossed. Stand up from and sit down slowly onto a chair (this can be made easier and more difficult by changing the height of the chair). Repeat 10 times. 2 to 3 sets.
Passive Knee Extension

When sitting place your operated leg out in front of you. If you are on a bed or sofa then place cushions or a rolled-up towel under your heel so the back of the knee is not supported. This can also be achieved with the foot on a foot stool or chair and the knee unsupported.
Place your hand above the knee cap and apply pressure to the front of your knee pushing the leg straight. Hold for 20 seconds and repeat 4 times every few hours during the day.
Extension Holds
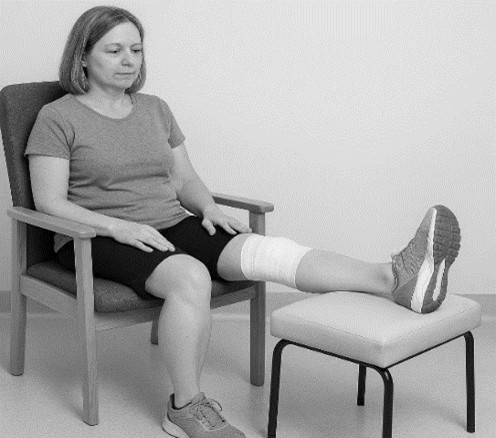
On an evening you should aim to sit in this position and hold it for a sustained time of about 60 minutes. You can do this whilst icing the knee, watching TV or before you go to bed. If the knee aches holding it for this length of time, then you may bend it a few times every now and then to release the tension, then go back into this position until the hour is completed.
Contact Information
University Hospital of North Tees
Orthopaedic Outpatients
Telephone: 01642 383838
Email: [email protected]
Monday to Friday, 9:00am to 4:00pm
Physiotherapy Admins
Telephone: 01429 522471
Website: https://www.nth.nhs.uk/services/trauma-orthopaedics/lower-limb/
Monday to Friday, 9:00am to 4:00pm
If you have any immediate concerns outside of these hours, please contact 111 or attend your local Urgent Care Centre/Minor Injuries Unit.
Information for Patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
Patient Experience Team (PET)
North Tees and Hartlepool NHS Foundation Trust would like your feedback. If you would like to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Team who will help you to do this.
This service is based at the University Hospital of North Tees but also covers The University Hospital of Hartlepool, our community hospitals and community health services.
North Tees and Hartlepool NHS Foundation Trust
Telephone: 01642 624719
Freephone: 0800 092 0084
Email: [email protected]
Monday to Friday, 9:30 am to 4:00 pm
Out of Hours
If you wish to speak to a senior member of Trust staff, please contact the hospital switchboard (numbers below).
| University Hospital of North Tees | University Hospital of Hartlepool |
| Hardwick Road Stockton-On-Tees TS19 8PE Telephone: 01642 617617 | Holdforth Road Hartlepool TS24 9AH Telephone: 01642 617617 |
Leaflet Reference: PI024 – Version 01
Review Date: 16/03/2029