Information for patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
This leaflet describes why you are having an Endoscopic Ultrasound (EUS) Guided Coeliac Plexus Block procedure and what it involves.
Please read this leaflet carefully before coming for the procedure so that you can ask any questions you may have when you attend.
You will be asked to sign the consent form after you have had a chance to ask questions.
What is an Endoscopic Ultrasound (EUS) Guided Coeliac Plexus Block?
You have been advised to have an EUS.
This is a procedure that allows an Endoscopist (a consultant trained to do EUS) to see inside your oesophagus (gullet or food pipe), stomach and duodenum (small intestine) and the organs outside it (liver, pancreas, gall bladder, kidneys, adrenal glands, lymph glands, blood vessels and nerves) using an EUS endoscope. (See diagram below).
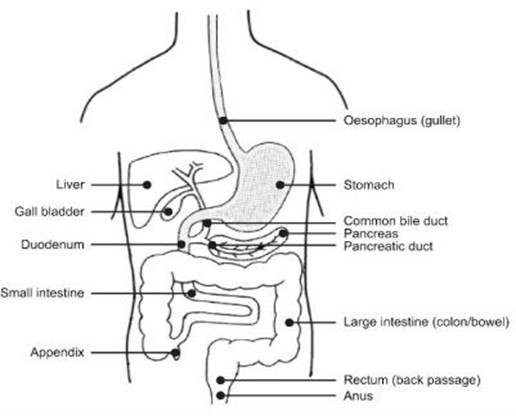
An EUS endoscope (a thin, flexible tube with a bright light and small ultrasound probe on the end), will be passed through your mouth and down into your stomach and small bowel.
Once the EUS endoscope is in position, ultrasound waves are used to see the area and structures deeper in the chest and abdomen.
Your doctor has requested to carry out EUS Guided Coeliac Plexus block to help with your pain symptoms. This will be explained to you in more detail before the procedure. You will need to have a blood test before the procedure to check that your blood is clotting properly.
What is the Coeliac Plexus?
This is a bundle of nerves that come together. They send out pain signals through your nerves to organs such as your liver, pancreas and others.
The coeliac plexus is close to the spine at the level of your tummy button.
This procedure blocks the coeliac plexus by injection of local anaesthetic and steroids around it. The result is that the nerves can no longer send pain signals to the brain resulting in relief from abdominal pain.
Who is this procedure for?
This procedure is only for patients with uncontrollable abdominal pain, patients suffering from pancreatic cancer and some people with chronic pancreatitis.
Why am I having this procedure?
Your doctor has referred you for this procedure because you have upper abdominal pain that is not helped by taking medicines.
By blocking the coeliac plexus, we expect the feeling of pain to improve for two to three months for between 5 to 8 people out of every 10 people. This procedure can be repeated if the pain comes back after this time.
For some people, pain might completely stop and sometimes it can help other symptoms such as nausea (feeling sick).
What are the risk and possible complications?
Most EUS & coeliac plexus block procedures are straightforward. However, there is a small chance that you may have side effects or complications. These include:
• Damage to your teeth or bridge-work – The EUS endoscope can occasionally cause damage to your teeth or bridge-work. This is rare and a mouth-guard is used to lower the risk.
• Aspiration – If you are sedated and your stomach contains food or drink, it can leak into your lungs. This can affect your breathing and cause an infection. This is why you must not eat or drink for 6 hours before the procedure.
• Bleeding – If any bleeding happens during your procedure, steps will be taken to stop it. You may need a blood transfusion, or rarely, an operation. This can happen to 2 patients in every 100.
• Perforation (a hole or tear in the gullet or stomach) – Depending on the type of EUS procedure, this can happen to 1 patient in 500. If this happens, this will need treatment with fluids, antibiotics and sometimes surgery.
• Pancreatitis (inflammation of the pancreas gland leading to abdominal pain, vomiting and fever) – This is rare and it may happen if a biopsy or a fine needle aspiration (FNA – a sample of cells taken from your pancreatic tissue) has been taken from the pancreatic tissue.
If this happens, you would need to stay in hospital for a few days to receive intravenous fluids and pain relief. This can happen to 2 patients in every 100.
• Hypotension (low blood pressure) – This may happen for a short time following the coeliac plexus block. To help prevent hypotension, you will be given some intravenous fluids (a drip) immediately following your procedure. This can happen to 5 patients in every 100.¹
• Diarrhoea – This may happen temporarily following coeliac plexus block and will
usually stop without medication. This can happen to 28 patients in every 100.1
• Post-procedural pain & exacerbation of existing pain – This may happen temporarily and usually lasts for less than 48 hours. This can happen to 9 patients out of every 100.
• Infection – Although rare, this can happen following coeliac plexus block. Once diagnosed, it is usually treated with antibiotics.
• Paraplegia – This is a type of paralysis that affects your ability to move the lower half of your body. This is extremely rare.
• Diaphragmatic paralysis – This is a condition in which your diaphragm (a muscle below your chest that helps you to breathe) is unable to contract. This stops proper inspiration (breathing in movement). This is extremely rare.
• Adverse effects of conscious sedation (a drug which should make you feel
comfortable and relaxed) – This can occasionally cause problems with your breathing, heart rate and blood pressure. Careful monitoring (checking) by a fully trained endoscopy Nurse will make sure they are identified and treated quickly.
• Ischaemia – This is extremely rare which may result in ischaemic damage (not getting enough blood) to nearby organs.
Severe complications are rare, but may require emergency admission, repeat endoscopic procedure, surgery, blood transfusion or, in extremely rare circumstances, result in death.
Are there any other procedures that can be done instead of having a coeliac plexus block?
You do not have to have any procedures you do not want, but the Doctor who has requested the treatment has advised this is best for you.
Your consultant has recommended this procedure as being the best option. There are no alternative procedures available.
What will happen before my procedure?
You will be admitted as a day case patient on the morning of your procedure, unless your appointment letter states otherwise.
You will usually be able to go home on the same day of your procedure. Very occasionally, your doctor may advise you to stay in hospital overnight. The reasons for this will be explained to you.
What will I need to do to prepare for my procedure?
It is very important you follow the instructions given in this leaflet to make sure your oesophagus (food pipe), stomach and duodenum (intestine, gut) are empty. This will allow the Endoscopist to get a clear view and make sure no areas are hidden.
You must stop eating or drinking at least 6 hours before your procedure. This is very important. You must follow the instructions. Nothing means nothing at all.
If you forget and you do eat or drink anything, you must tell your doctor or Nurse, as your procedure may need to be delayed for your safety. This is because when you are sedated, if your stomach contains food or drink and you vomit (throw up), it could get into your lungs, affect your breathing and cause an infection.
If you are taking any medication to thin your blood or if you are unsure, you must contact the Endoscopy Unit as soon as you get your appointment.
This medication includes anticoagulants such as Warfarin, Apixaban, Dabigatran, Rivaroxban amongst others, or antiplatelet medications such as Aspirin, Clopidogrel, Ticagrelor, Dipyridamole amongst others.
You can continue to take Aspirin if you are already doing so, but you must stop taking this on the morning of your procedure. If you have diabetes, you should contact the Endoscopy Unit for advice about your medication.
Can I be sedated for the procedure?
Yes, the effect of sedation will stay with you for at least 24 hours so it is important you follow this advice.
Under rare circumstances, we can do the procedure without sedation. This can mean that the procedure might become slightly uncomfortable.
There must be a responsible adult to take you home and look after you for the first 24 hours after your procedure. This is because the effects of the sedation will affect your judgement.
For the first 24 hours after sedation you:
• Must not go back to work.
• Must not drive a car, ride a bicycle or motorcycle. It is an offence to drive while unfit to do so because of drugs and it will probably invalidate your insurance policy.
• Must not supervise children.
• Must not make important decisions or sign any legal documents.
• Must not operate machinery or electrical appliances.
• Must not go near open flames or sources of high heat.
• Must not drink alcohol.
• Must not take sleeping tablets, tranquillisers or any drugs other than those prescribed for you by your GP.
• Must not lock the toilet or bathroom door in case you need any help.
• Should not smoke.
If you have not arranged for somebody to look after you, you will not be able to be sedated and your procedure will have to be postponed.
What will happen when I arrive for my appointment?
When you arrive at the Endoscopy Unit, you will be advised by the Endoscopy Nurse of an approximate time you should be ready to go home. Anyone wishing to stay and wait for you will be taken to an area where they can wait.
There is limited space in the Unit, so only in special cases will someone be allowed to stay with you, for example, adults with special needs.
A Nurse will call you through to the Unit. They will check your personal details and ask you questions about your health.
They will also check your blood pressure and pulse and explain the procedure and risks to you. This is to make sure you understand everything before you sign the consent form.
You should tell the Nurse if you have had any allergies or reactions to drugs or other procedures in the past. You should also tell your Nurse about any previous endoscopy procedures you may have had.
Please bring with you a list of medications (drugs) you are currently taking. This includes medicine prescribed by your doctor or those you have bought yourself.
You will be asked for a contact telephone number of the relative or friend who will take you home and stay with you after your EUS.
You will be taken to a comfortable waiting area to wait your turn. We operate a list system. This means you will be seen when it is your turn and not the time given for you to arrive at the unit.
Before your examination, if you have any worries or questions, please talk to your Nurse or Endoscopist.
What should I do on the day of my procedure?
On the day of your procedure, it is important that:
• You do not smoke.
• Long hair should be tied back for comfort.
• You avoid bringing valuables with you.
• You wear loose fitting clothing.
• False teeth, glasses and hearing aids may be removed in the Endoscopy Room.
When it is time for your procedure, a Nurse will take you into the examination room.
What will happen during my procedure?
Before your procedure begins, you will be asked to remove any false teeth, if you have them. A local anaesthetic will be sprayed on to the back of your throat to numb the area.
You will be given a sedative drug before the examination starts. This is called conscious sedation. You will still be awake but should feel more comfortable and relaxed.
This involves injecting medication (drugs) through a cannula (a fine tube) inserted into a vein in the back of your hand or arm using a small fine needle.
In the examination room, you will then be asked to lie down on a trolley on your left side. Your pulse, blood pressure and oxygen levels in your blood will be checked before and during your procedure by putting a small plastic clip on to one of your fingers. A nurse will make sure you are comfortable and your privacy and dignity will be maintained at all times throughout the procedure.
You will be given extra oxygen to breathe through a soft plastic tube on your nose. A small plastic guard will be put gently between your teeth to protect them. Do not worry, this is all routine and is not painful.
The Endoscopist will then pass the EUS scope through your mouth, into your stomach and then into your duodenum (gut). Air will be passed through the tube to inflate your stomach so that your Endoscopist can see all parts of your stomach wall. This can cause “windy” discomfort. The coeliac plexus block will then be carried out.
During the procedure, any extra saliva will be cleared from your mouth using a fine suction tube. When the procedure is over, the air and the EUS camera are removed quickly and easily.
We routinely take photographs or videos of your insides during this procedure. These are used to help in your investigations and treatment.
The procedure may take up between 45 to 60 minutes to be completed.
What happens to the pictures taken during my procedure?
The pictures taken during your procedure will be kept as part of your healthcare record. These may sometimes be used anonymously for training or research.
If hospital staff want to use any of your pictures for any other purpose, for example, in an article to be published (printed) in a professional magazine or book, they will ask your permission before this happens.
What will happen after the procedure?
You will be taken to the recovery area where you will be able to rest on a trolley until the immediate effects of the sedation have worn off.
You will be given some fluids through the intravenous cannula (drip) to prevent hypotension (low blood pressure).
You will usually be able to go home on the same day of your procedure.
The person you have arranged to take you home will then be asked to come onto the Unit to collect you. You will not be able to go home on your own. Occasionally your doctor may advise you to stay in hospital overnight.
Will my pain improve after having this procedure?
Not all people will get complete pain relief all the time. However, we expect that the majority of patients having this procedure will find some benefit.
Some people will have complete easing of their pain and others will notice improvement and will be less reliant on painkillers.
This tends to happen gradually over the first week or so after the procedure in most people, while some others find the pain goes away straight away.
Can Coeliac Plexus Block be repeated?
Generally, we expect relief of pain symptoms to last for 2 to 3 months after this procedure. If your pain was eased after your procedure but then comes back and cannot be controlled with painkillers, then the procedure may be repeated.
Should I take any special precautions after the procedure?
You might feel slightly more under the weather for the first 24 to 48 hours after your procedure. We recommend that you get plenty of rest during this time. Because of the sedation given for the procedure, you will not be able to drive or operate heavy machinery for 24 hours.
What follow-up is planned after my procedure?
A copy of the report will go to your referring team who will continue to manage your symptoms.
When will I be told about the outcome of my procedure?
Before you leave the unit, your Nurse or Endoscopist will explain the outcome of your procedure to you. A copy of your report will be sent to your GP within 24 hours.
If you are an inpatient, the outcome of the procedure will be discussed with you on the ward by the Doctor responsible for your care.
Contact Number
If you need further advice, or have any problems, please contact the Unit where you are to have your examination.
University Hospital of North Tees
Endoscopy Unit
Telephone: 01642 624387
Monday to Saturday, 8:00 am to 7:00 pm
Emergency Department
Telephone: 01642 382899
24 hours a day, 7 days a week
Reference
1. Adverse events associated with EUS and EUS-guided Procedures, Nauzer Forbes, Nayantara Coelho-Prabhu, Mohammad A. Al-Haddad et al, ASGE Standards of Practice Committee, Gastrointestinal Endoscopy Volume 95, No. 1, 2022.
2. Endoscopic ultrasonography guided celiac plexus neurolysis and celiac plexus block in the management of pain due to pancreatic cancer and chronic pancreatitis, Anthony J Michaels, Peter V Draganov, World Journal of Gastroenterology ISSN 1007- 9327, July 2007.
Comments, concerns, compliments or complaints
Patient Experience Team (PET)
North Tees and Hartlepool NHS Foundation Trust would like your feedback. If you would like to share your experience about your care and treatment or on behalf of a patient, please contact The Patient Experience Team who will help you to do this.
This service is based at the University Hospital of North Tees but also covers the University Hospital of Hartlepool, our community hospitals and community health services.
North Tees and Hartlepool NHS Foundation Trust
Telephone: 01642 624719
Freephone: 0800 092 0084
Email: [email protected]
Monday to Friday, 9:30 am to 4:00 pm
Out of Hours
If you wish to speak to a senior member of Trust staff, please contact the hospital switchboard.
Telephone: 01642 617617
Leaflet reference: PI026 – Version 01
Date for Review: 16/01/2029