Information for patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
Introduction
This leaflet explains why you have been referred for a total knee replacement operation.
The orthopedics team are here to assist you with all of your needs, and we will provide you with advice and guidance.
Please do not hesitate to ask any member of the tea if you have any questions or concerns at any time.
What is a knee replacement?
The knee is a hinge joint. It is at the bottom of your femur (thigh bone) and the top of your tibia (shin bone). During the operation, the worn or damaged joint will be replaced with an artificial joint.
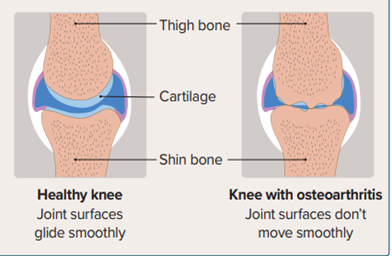
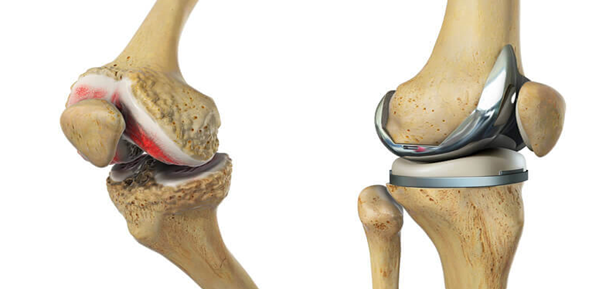
What are the benefits of surgery/
A knee replacement is usually carried out because of severe pain and restricted movement. These can limit activity and lifestyle choices.
A knee replacement may provide benefits such as:
What are the associated risks?
Knee replacements are generally very successful, and patients can gain an improved lifestyle benefit. It lasts for an average of 25 years. There is, however, a risk of complications. These can include:
What happens before your surgery?
You will be invited to attend and education class. This is an important part of your journey, to provide you with information you need to make the best of your health before your operation, and to aid your recovery after that.
You will meet the joint replacement specialist nurse and physiotherapist, you will learn about your care, rehabilitation and what is expected of you before and after your surgery.
We will discuss your anaesthetic, talk about medications and pain relief. We will show you a model of a total knee replacement and trach you exercises you need to perform before and after surgery.
You will also have a final appointment with the specialist nurse approximately 2 to 3 weeks before your operation/admission.
During this clinic visit, you will have simple tests on your heart and lungs and may need a repeat blood test taken. Bring a urine sample with you (using the bottle provided at your education class) This will be tested to rule out infection. You may require repeat X-rays.
You will be given body wash and nasal ointment to use 5 days before your operation. This is to help prevent MRSA infection.
You will need to bring with you a list of all medications you take or a repeat prescription. We will discuss with you any medications that you may need to stop before your operation date.
What if I need help at home?
You can discuss this with the occupational therapist, who can arrange for carers to be put in place for your discharge.
You will also be given a form on your final check appointment before surgery that will ask you questions regarding equipment that may be needed for your return home.
This will all be explained to you by the joint replacement specialist nurse. Your equipment will be delivered prior to your operation.
How should I prepare for my admission to hospital?
Please ensure you have a bath or shower before you arrive at the hospital to aid in the prevention of the risk of infection.
It is also important that you do not apply creams or make up after your bath or shower.
Please do not shave your legs for at least 3 weeks prior to your operation. Shaving is known to increase infection rates in joint replacement. It is not know whether hair removal creams increase infection risks so these may be best avoided.
What should I bring to hospital for my admission?
You should bring well fitting, comfortable slippers or flat supportive shoes to walk in. New slippers may not fit if your feet become swollen, and slippers/shoes without a back are not recommended.
You should also bring easy fitting clothes.
You must bring any medication normally prescribed by your own doctor, or any over the counter medications with you on admission. Please bring them in their original packets. Any medication that is not in its original pack cannot be used on the ward.
Please bring in any leaflets, walking aids, and equipment provided to you for the operation. For example, a helping hand, show horn, or sock aid.
Please only bring essentials into hospital as there is only limited space and no suitable storage for valuables.
What happens during my admission to hospital?
You will be admitted to hospital on the day of your procedure. You will be given a time slot, which is designed to make your stay in hospital before the operation as short as possible. You’ll be admitted to the access lounge, where all of the checks will be completed before you go into theatre.
When you are admitted to the access lounge you will be seen by an anaesthetist, who will discuss your anaesthetic choices with you.
Most patients will be recommended to have a spinal anaesthetic, in combination with a light general anaesthetic or sedation.
The spinal anaesthetic involves a small injection of local anaesthetic between the bones of the lower part of the back, around the nerves of the spinal cord. This causes a temporary numbness and heaviness from the waist down and allows surgery to proceed without you feeling any pain.
Light general anaesthesia or sedation may then be given to reduce your awareness of theatre activity during surgery. This anaesthetic combination is preferred because it is safe, effective and its full effects usually wear off very quickly following surgery.
This allows most patients to make a rapid recovery with few hangover side effects. It will also allow and promote early mobilisation.
Other anaesthetic choices include: General anaesthesia and/or combined with nerve block or epidural anaesthetic. An epidural anaesthetic is similar to a spinal anaesthetic, but it can be continued after surgery in the ward.
Your anaesthetist will discuss the pros and cons of these choices with you.
From the start of the anaesthetic until the end of your operation, your anaesthetist will stay with you, watching your condition very closely.
Your heart rate, blood pressure and breathing are monitored throughout and your body temperature is kept normal using a warming blanket.
As with all anaesthetic techniques, there is the possibility of side-effects or complications with a spinal anaesthetic.
Common side effects include:
Rare side effects:
What happens during the operation?
you should be aware that in theatre the operating team wear specialist clothing, hoods and masks, this is to further minimise the risk of infection.
At the end of the operation, the surgeon will inject local anaesthetic into the tissues around the new joint which will assist to relieve your pain.
What happens following the operation?
You will go into the recovery unit. The staff will check your general condition, take observations of your pulse, blood pressure, temperature (vital signs), check your wound, monitor the reversals of your spinal anaesthetic, and assess if you need any further pain relief.
Once the anaesthetist is happy with your recovery and vital signs, you will return to the elective care unit where the staff will continue to monitor your vital signs, bladder and bowel functions, the return of feeling in your legs and lower body following the spinal anaesthetic.
You will have regular pain relief prescribed. If you feel your pain relief is inadequate at any time then you must let the ward nurses know so that they can help you get more comfortable, and provide you with medication required.
You will be encouraged to be as independent as possible. You will be expected to get dressed into your normal clothes. A physiotherapist/occupational therapist will visit you daily on the ward.
It is important that you exercise independently at times through the day when the physiotherapist is not attending you.
You will be escorted to X-ray to have imaging taken of your knee replacement. Blood tests will also be taken on this day.
You will be encouraged to attend your own personal hygiene with minimal assistance. It is important that you continue with your physiotherapist exercises, and learn how to walk with a Zimmer frame before progressing to elbow crutches or walking sticks. You will also practice stair climbing if necessary.
The nursing staff will discuss your discharge plan with you as soon as possible after your operation, to ensure you have all of the necessary equipment and help in place at home before you leave the ward.
You will be discharged home when you are medically fir and have completed all of your physiotherapy and occupational therapy assessments.
Will my medication change following surgery?
You will be prescribed some new medicines. Some are to help to reduce the amount of pain, and some help to reduce the risks of complications following surgery. There may also be some temporary changes to your regular medicine, but if there is it will be explained to you.
The nursing staff will give you your medication prior to you leaving the ward. You will be discharged from hospital with 1 week supply of tablets to relieve the pain, and you will need to contact your GP for any further prescriptions required.
Before you leave the ward you will be given a discharge letter. This contains information about your operation and medication. Your GP will receive a copy of this letter on the day you are discharged.
What happens following discharge home?
A few days after you have been discharged, you will be contacted by a member of the joint replacement specialist nurses team to see how you are getting on.
Your wound review appointment will be carried out approximately 2 weeks after surgery, this will be given yo you at your final pre-op appointment with the joint replacement nurses.
You will have a consultant or a joint replacement specialist nurse review around 6 to 8 weeks after surgery to check your progression.
You will be reviewed again at 5 months in a virtual clinic (phone call appointment), and asked to attend for an X-ray at a convenient time.
There will also be a review at 1 year and you will be asked to attend for an X-ray. If you have met all required milestones you will then be discharged back to the care of your GP.
If you have concerns regarding your recovery, or think you may be developing a problem please contact the helplines (listed in the back of this leaflet). We will be able to offer advice and arrange additional support, or organise a review if required.
How to care for your wound
Your wound may leak slightly into your dressing and dry up. This is normal, if it leaks outside of the dressing you must contact the service straight away (numbers provided in the back of this booklet). Your wound dressing should remain in place for at least 14 days.
You will attend an outpatient appointment for this with the joint replacement specialist nurse, given to you prior to surgery.
Your dressing will only be changed if the dressing will not stay in place of attach to your skin.
Please do not change the dressing yourself.
The dressing on your knee wound has a bacterial barrier to help reduce the risk of infection, it is not advisable to shower for at least 14 days after surgery. Washes only are advised.
An infection at the site of your wound is unusual but may present with discharge from the wound, redness, swelling and heat, increased pain or an offensive smell. You must seek advice from the helpline number or contact the ward where you had your surgery.
If you are concerned about your wound, please call the helpline at any time.
If your GP or district nurse prescribes antibiotics for a possible wound infection, please contact the joint replacement specialist nurses, we may need to arrange an appointment with your surgeon.
Seek advice from your hospital or GP if you notice any excessive bleeding, or any difficulty with breathing. If you become urgently unwell, call an ambulance.
Frequently Asked Questions
References
NJR (National Joint Registry)
NIHR (National Institute for Health and Care Research)
NICE (The National Institute for Health and Care Excellence)
Contact Numbers
Joint replacement specialist nurses
Monday to Friday: 8.30am to 4.30pm
Hartlepool
Telephone: 01429 522493
Ward 4 Hartlepool
Telephone: 01642 382804
Physiotherapy Ward 4 Hartlepool
Telephone: 01429 522030
Ward 32 North Tees
Telephone: 01642 382732
Ward 33 North Tees
Telephone: 01642 382733
Returning Equipment
Durham and surrounding districts
Telephone: 01325 524531
TCES Equipment Hartlepool, Stockton and Middlesbrough
Telephone: 01642 224205
Comments, concerns, compliments or complaints
Patient Experience Team (PET)
We are continually trying to improve the services we provide. We want to know what we’re doing well or if there’s anything which we can improve, that’s why the Patient Experience Team (PET) is here to help. Our Patient Experience Team is here to try to resolve your concerns as quickly as possible. The office is based on the ground floor at the University Hospital of North Tees if you wish to discuss concerns in person. If you would like to contact or request a copy of our PET leaflet, please contact:
Telephone: 01642 624719
Freephone: 0800 092 0084
Opening hours: Monday to Friday, 9:30am to 4:00pm
Email: [email protected]
Out of hours
Out of hours if you wish to speak to a senior member of Trust staff, please contact the hospital switchboard who will bleep the appropriate person.
Telephone: 01642 617617
Data protection and use of patient information
The Trust has developed Data Protection policies in accordance with Data Protection Legislation (UK General Data Protection Regulations and Data Protection Act 2018) and the Freedom of Information Act 2000. All of our staff respect these policies and confidentiality is adhered to at all times. If you require further information on how we process your information please see our Privacy Notices.
Telephone: 01642 383551
Email: [email protected]
Privacy NoticesLeaflet feedback
This leaflet has been produced in partnership with patients and carers. All patient leaflets are regularly reviewed, and any suggestions you have as to how it may be improved are extremely valuable. Please write to the Clinical Governance team, North Tees and Hartlepool NHS Foundation Trust, University Hospital of North Tees, TS19 8PE or:
Email: [email protected]
Leaflet reference: PIL1462
Date for Review: September 2026