Information for patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
Your doctor has advised you have a flexible sigmoidoscopy:
- To help find the cause of your symptoms.
- As part of a routine screening programme to detect (find) disease or abnormalities (unusual areas) at an early stage in people with no symptoms.
- To follow up previous abnormalities.
This leaflet tells you about flexible sigmoidoscopy and will help you understand what will happen during and after your examination.
What is a flexible sigmoidoscopy?
A flexible sigmoidoscopy is an examination that allows an endoscopist (a doctor, nurse or physician associate trained to do endoscopies) to see inside your large intestine (bowel or colon). This is the most accurate way of looking inside your bowel. The procedure includes a rectal examination, in which the endoscopist uses their finger to assess for any abnormalities inside your bottom back passage (rectum) before inserting the scope. The rectal examination is usually very quick and should not cause you too much discomfort.
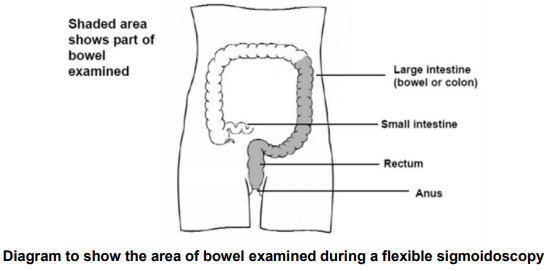
A flexible sigmoidoscope (a soft, flexible tube about the thickness of a finger) is passed into your rectum (back passage) and guided through the lower part of your large intestine (see diagram on the next page).
The flexible sigmoidoscope has a bright light and camera at the end that passes back pictures of the inside of your bowel onto a monitor.
Your endoscopist can then check if any disease or abnormalities are present. Biopsies (small pieces of tissue) can be taken and any polyps (small wart-like growths) can be removed for examination in a laboratory.
If any abnormality is found during the sigmoidoscopy your endoscopist may need to examine higher up your large bowel (a colonoscopy), to make sure there are no other abnormalities.
What are the risks and possible complications?
Flexible sigmoidoscopy is a safe examination, but does have some risks and possible complications. These will be discussed fully before you consent to the examination. They must be compared to the benefits of having the examination carried out. The doctor who advised you to have this examination will have considered this.
The risks and possible complications include:
- Discomfort. You may feel some discomfort during the examination; we try to keep this to a minimum. You can ask for the procedure to stop at any point if you wish.
- Bloating. You may feel bloated for a few hours afterwards.
- Rectal bleeding. 1 patient in every 3862 can suffer rectal bleeding. This may need a blood transfusion, or rarely, an operation. The risk can increase if polyps are removed. If the bleeding happens during the test the endoscopist will try to stop the bleeding with clips and injections. Sometimes bleeding can occur up to 2 weeks after the procedure
- Perforation (hole). 1 patient in every 2,5112 can suffer a perforation in the wall of the bowel. The risk of perforation is higher with polyp removal. This can happen to 1 patient in every 100 when large or complex polyps are removed. If a perforation happens, sometimes the hole can be closed with clips during the colonoscopy. If the hole cannot be closed an emergency operation is needed to repair it.
Sometimes, during the operation, a stoma (opening where the end of your bowel is brought out on to the skin of your abdomen (tummy) may be needed to allow your bowel to rest and heal. The stoma can usually be closed when your bowel has healed. - Conscious sedation. (A drug which makes you feel comfortable and relaxed). This can occasionally cause problems with your breathing, heart rate and blood pressure. Careful monitoring (checking) by a fully trained endoscopy nurse will make sure any problems are identified and treated quickly.
- Incomplete test. There is also a possibility that the procedure will be incomplete and that some part of your large intestine will not be examined as intended. In this case, your endoscopist or referring doctor will discuss alternative tests with you.
- Missed lesions. Flexible sigmoidoscopy is a very accurate examination but occasionally an abnormality (including, rarely, a cancer) may be missed4,5,6.
- Other treatments. If any biopsies or polyps are removed, the risks can increase.
Are there any other tests that can be done instead of a flexible sigmoidoscopy?
You do not have to have any examination or tests you do not want, but the doctor who has requested the examination has advised this is best for you. If you do not want this examination, a CT scan could help to find the cause of your symptoms. However, these are not always as clear as a flexible sigmoidoscopy.
If you decide not to have a flexible sigmoidoscopy you will need to let the Endoscopy Unit know before your appointment date.
If you decide you want a CT scan instead, you will need to go back to your GP surgery/referring Doctor to discuss the options available.
What will happen before my flexible sigmoidoscopy?
You will be admitted as a day case patient unless your appointment letter states otherwise. You will usually be able to go home 15 – 30 minutes after your examination. Very occasionally, your doctor may advise you to stay in hospital overnight after your flexible sigmoidoscopy.
Flexible sigmoidoscopy is usually done without any sedation. If sedation is requested this will be given to you before your examination begins. This is called conscious sedation. You will still be awake but should feel more comfortable and relaxed. This involves injecting medication (drugs), through a cannula (a fine tube) inserted into a vein in the back of your hand or arm using a small, fine needle. If you have sedation you may have to stay in the unit a little longer.
What will I need to do to prepare for my flexible sigmoidoscopy?
It is very important that your bowel is empty and clean or certain areas of your bowel will be hidden and your flexible sigmoidoscopy may have to be rearranged. You must follow the instructions given in the leaflet, ‘How to prepare for a colonoscopy or flexible sigmoidoscopy – Moviprep‘.
Occasionally, a flexible sigmoidoscopy may be performed with Enema preparation only. This is, typically, specifically requested by your Consultant/GP and discussed with you at the time your referral is decided.
The enema is delivered through your rectum (back passage) via a soft plastic nozzle attached to a squeezable bottle. Typically, you will be asked to lie on your left side with knees drawn up for ease of administration. The solution usually works within 5 to 10 minutes, producing a bowel movement. Enemas are usually safe and do not cause any complications. However, on very rare occasions, the nozzle may cause a hole/tear (perforation) in the wall of your rectum. If a perforation occurs, you may need admission for monitoring and, occasionally, surgery to repair the hole and clean any leaked content to prevent infection.
If you request sedation you must arrange for a responsible adult to take you home and stay with you for at least 12 hours after your examination as the effects of the sedation will affect your judgement. If you have not made these arrangements and want to be sedated your flexible sigmoidoscopy will have to be postponed.
Please bring a dressing gown, slippers or flat shoes, a list of medications (drugs) you are currently taking, either prescribed by your doctor or those you have brought yourself and your reading glasses with you on the day of your appointment.
What will happen when I arrive for my appointment?
When you arrive at the Endoscopy Unit you will be told the approximate time you should be ready to go home. Anyone wishing to stay and wait for you will be shown where they can wait. There is limited space in the unit, so only in special cases will anyone be able to stay with you, for example, parents with children or adults with special needs.
A nurse will call you through to the unit, check your personal details, ask you questions about your health, check your blood pressure and pulse and explain the examination to you. This is just to make sure you understand everything before you sign the consent form. You should tell the nurse if you have any allergies or have had reactions to drugs or other tests in the past and of any previous flexible sigmoidoscopies or colonoscopies you may have had. We operate a list system, this means you will be seen when it is your turn and not the time given for you to arrive at the unit.
Before your examination you will be taken to a private area and asked to undress. You will be given a gown and some modesty pants to put on, together with your dressing gown and slippers.
You may be taken to a waiting area with other patients to wait your turn. When it is time for your flexible sigmoidoscopy a nurse will take you into the examination room. Your nurse or endoscopist will explain the examination again and discuss the risks described earlier. If you have any questions or concerns, please talk to your nurse or endoscopist.
What will happen during my examination?
Before your examination begins, if you have requested sedation a cannula will be inserted into a vein in the back of your hand or arm using a small, fine needle. The sedative drugs will be given through the cannula just before your examination begins. This should help you to feel more comfortable and relaxed.
You will be asked to lie down on a trolley on your left side, with your knees slightly bent. A small plastic clip will be put on to one of your fingers to check your pulse and the oxygen levels in your blood, before and during your examination. You may be given extra oxygen to breathe through a soft plastic tube on your nose. Do not worry, this is all routine.
A nurse will stay with you during your examination and make sure you are comfortable. The flexible sigmoidoscope will then be gently inserted into your rectum and guided through your large bowel. Air will be passed through the tube to inflate your bowel so your endoscopist can see all parts of your bowel wall. This can cause ‘windy’ discomfort. You may feel you want to open your bowels but as they are already empty this will not happen.
The examination can take from 5 – 20 minutes to complete.
We routinely take photographs or videos of your insides during this examination. These are used to help in your investigations and treatment. The pictures taken during your examination will be kept as part of your healthcare record.
The pictures may sometimes be used for training or research but would always be anonymised (they would have no details which could identify you). If hospital staff want to use any of your pictures for any other purpose, for example, in an article to be published (printed) in a professional magazine or book, they will ask your permission before this happens.
Will it be painful?
Usually this examination is not painful, but you may feel some discomfort. If needed, you can be given a special gas called Entonox to breathe. You can ask for the examination to stop at any point if you wish.
What will happen after my examination?
If you have not had sedation you will be taken to a private area to get dressed. You will be offered a drink and a snack before you go home. You will be given a leaflet ‘Flexible sigmoidoscopy without sedation – Discharge advice’ before you go home.
If you have had Entonox, you must not drive until 30 minutes after the procedure. You will be given a leaflet ‘Flexible sigmoidoscopy with Entonox – Discharge advice’ before you go home.
If you have had sedation you will be taken to the recovery area where you will be able to rest until the immediate effects of your sedation have worn off. After this you will be helped off the trolley and you can get dressed. You will then be offered a hot drink and a snack. The person you have arranged to take you home will be asked to come to the unit to collect you.
You will not be able to go home on your own. You will be given a leaflet ‘Colonoscopy or flexible sigmoidoscopy with sedation – Discharge advice’ before you go home.
When will I be told the results of my colonoscopy or flexible sigmoidoscopy examination?
Before you leave the unit your nurse or endoscopist will explain the results of your examination to you and you will be given a copy of this. Your GP will be sent a report.
If the endoscopist who has done your endoscopy feels it is necessary, you may be given some medication and/or an outpatient appointment.
If you had any biopsies taken and sent to a laboratory for further examination you may have to wait for up to 6 weeks for the results. Your GP will also be sent a copy of these results. If you are given an outpatient appointment, your results will be discussed with you then. If you have not received your results, you can make an appointment to see your GP to discuss them. Please note the Endoscopy Unit do not receive a copy of your results.
Contact numbers
If you need further advice or have any problems, please contact the appropriate number below:
University Hospital of North Tees
Endoscopy Unit
Telephone: 01642 624387
Monday to Friday 8am to 7pm
Accident and Emergency Department
Telephone: 01642 382899
24 hours a day, 7 days a week
University Hospital of Hartlepool
Rutherford Morison Unit
Telephone: 01429 522356
Monday to Friday 8am to 6.30pm
If you have any worries or concerns you should contact your GP during normal surgery hours. Outside surgery hours you should contact your GP’s surgery for the Out of Hours Service number.
Further information is available from
NHS Choices telephone: 111 (when it is less urgent than 999)
Calls to this number are free from a landline and mobile phones via the website at www.nhs.uk
References
- Haycock, A., Cohen, J., Saunders, B., Cotton, P.B. and Williams, C.B. (2014). Cotton and Williams’ practical gastrointestinal endoscopy: the fundamentals. Chichester, West Sussex, Uk: John Wiley And Sons, Inc.
- Gavin D, Valori R, Anderson JT, et al. The National Colonoscopy Audit: a nationwide assessment of the quality and safety of colonoscopy in the UK. Gut 2013; 62:242–9
- Panteris V, Haringsma J, Kuipers EJ.Colonoscopy perforation rate, mechanism and outcome: from diagnostic to therapeutic colonoscopy. Endoscopy 2009;41:941-51.
- Burr, N.E., Derbyshire, E., Taylor, J., Whalley, S., Subramanian, V., Finan, P.J., Rutter, M.D., Valori, R. and Morris, E.J.A. (2019). Variation in post-colonoscopy colorectal cancer across colonoscopy providers in English National Health Service: population based cohort study. BMJ, [online] p.l6090. doi:https://doi.org/10.1136/bmj.l6090.
- Rutter, M.D., Beintaris, I., Valori, R., Chiu, H.M., Corley, D.A., Cuatrecasas, M., Dekker, E., Forsberg, A., Gore-Booth, J., Haug, U., Kaminski, M.F., Matsuda, T., Meijer, G.A., Morris, E., Plumb, A.A., Rabeneck, L., Robertson, D.J., Schoen, R.E., Singh, H. and Tinmouth, J. (2018). World Endoscopy Organization Consensus Statements on Post-Colonoscopy and Post-Imaging Colorectal Cancer. Gastroenterology, 155:(3), pp.909-925.e3. doi:https://doi.org/10.1053/j.gastro.2018.05.038.
- Morris, E.J.A., Rutter, M.D., Finan, P.J., Thomas, J.D. and Valori, R. (2014). Post-colonoscopy colorectal cancer (PCCRC) rates vary considerably depending on the method used to calculate them: a retrospective observational population-based study of PCCRC in the English National Health Service. Gut, 64:(8), pp.1248–1256. doi:https://doi.org/10.1136/gutjnl-2014-308362.
Comments, concerns, compliments or complaints
Patient Experience Team (PET)
We are continually trying to improve the services we provide. We want to know what we’re doing well or if there’s anything which we can improve, that’s why the Patient Experience Team (PET) is here to help. Our Patient Experience Team is here to try to resolve your concerns as quickly as possible. The office is based on the ground floor at the University Hospital of North Tees if you wish to discuss concerns in person. If you would like to contact or request a copy of our PET leaflet, please contact:
Telephone: 01642 624719
Freephone: 0800 092 0084
Opening hours: Monday to Friday, 9:30am to 4:00pm
Email: [email protected]
Out of hours
Out of hours if you wish to speak to a senior member of Trust staff, please contact the hospital switchboard who will bleep the appropriate person.
Telephone: 01642 617617
Data protection and use of patient information
The Trust has developed Data Protection policies in accordance with Data Protection Legislation (UK General Data Protection Regulations and Data Protection Act 2018) and the Freedom of Information Act 2000. All of our staff respect these policies and confidentiality is adhered to at all times. If you require further information on how we process your information please see our Privacy Notices.
Telephone: 01642 383551
Email: [email protected]
Privacy NoticesLeaflet feedback
This leaflet has been produced in partnership with patients and carers. All patient leaflets are regularly reviewed, and any suggestions you have as to how it may be improved are extremely valuable. Please write to the Clinical Governance team, North Tees and Hartlepool NHS Foundation Trust, University Hospital of North Tees, TS19 8PE or:
Email: [email protected]
Leaflet reference: PIL1437 version 1.1
Date for review: 12/07/2026