Information for patients
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
What is a pleural vent?
A pleural vent is a specially designed small tube to drain air from the space between the edge of the lung and the inside of the chest wall. The aim of the vent is to allow air to leave the space around your lung.
This system will allow your lung to return to its normal position. It is also designed to allow you to go home and be managed as an outpatient with the device still in place.
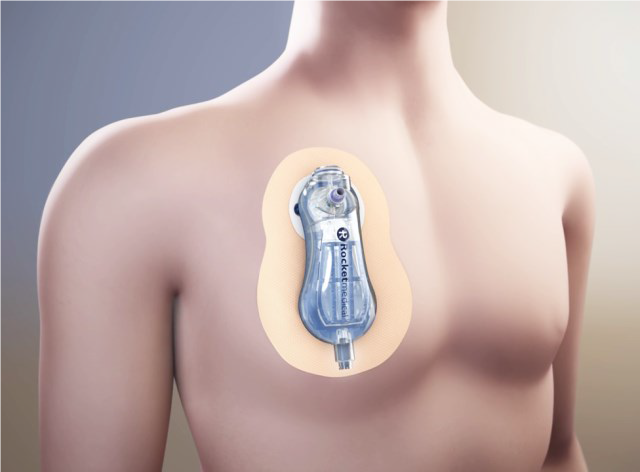
What is the benefit of a pleural vent?
When you breathe in, your lung follows the inside of your rib cage as it moves, but they are not stuck together. There is a double layered covering (the pleura), rather like ‘Cling Film’, between the outer surface of the lungs and the inside of the rib-cage. It is lubricated and allows the lungs to move with the rib cage when you breathe in and out.
In your case, air has built up between these layers and this is limiting how much your lung can expand. This is called a pneumothorax. This may be making you breathless.
Placing a pleural vent allows air to be removed to improve your breathing and makes it much more likely that you can safely go home today.
How is the procedure performed?
The doctor performing the procedure on the day will explain the whole process to you and ask you to sign a consent form. After this, the team will place you in a comfortable position, allowing the doctor access your chest. This involves asking you to lie on your back on a couch.
The procedure takes about 10 minutes and is performed by:
- Cleaning the site to kill any bacteria on your skin with an alcohol gel, which may feel cold.
- The doctor will then numb the area by injecting local anaesthetic in the skin and into the chest wall. A small needle is used for this which will feel sharp. You may feel a stinging sensation just before the anaesthetic starts working.
- Once the area is numb, the doctor will make one small cut in the numb area of the skin to create a path for the pleural vent. This should not be painful, though you may feel some pressure or tugging. The pleural vent is then gently positioned into the chest.
- A sticky back dressing attached to the pleural vent will be used to hold it in place on the front of your chest. Occasionally the doctor will use a stitch to hold it in place.
- A blue indicator button on top of the pleural vent should move up and down with your breathing. This shows that it is working.
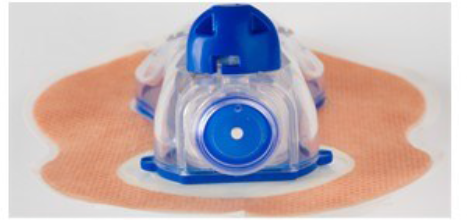
What happens after the procedure?
The nursing staff are very experienced and will look after you for the next hour. If you feel unwell in any way, please let the team know. You will have a chest X-ray and we may need to check your blood pressure during this time. The nurses will give you information on how to look after your pleural vent ambulatory system.
Provided that you are well and the chest X-ray shows that some of the air has been removed, you will be able to leave the hospital. Arrangements for clinical follow up in the lung department will be made before you leave.
What are the risks of a pleural vent?
Inserting a pleural vent is generally a routine and safe procedure. As with any medical procedure, there are potential risks which your doctor will explain. Some of these risks include:
- Some people get some discomfort during insertion. We will ensure you have pain killing medication to control this.
- Sometimes pleural vents can become infected but this is uncommon.
- Very rarely, a blood vessel can be damaged during insertion. This can cause significant bleeding, needing an operation to stop this. Our team is very experienced and try their best to avoid this.
- Very rarely the pleural vent may damage the lung and worsen the air leak (pneumothorax). Our team is very experienced and try their best to avoid this.
Aftercare Advice
This is a very safe procedure with few risks and it is rare for problems to occur.
If you develop pain which is not responding to standard painkillers or you develop increasing breathlessness in the hours after the procedure, you should contact the lung clinic (9am-5pm), or out-of-hours medical care (GP, ‘111’ service, or emergency services if you are feeling very unwell).
It is important to mobilise and breathe normally after the pleural vent is inserted, as this will help to drain the air. Occasionally, taking some deep breaths will also help.
You can shower with the Pleural Vent in place. However, you should try to keep the Pleural Vent and the dressing as dry as possible. The dressing will not be as effective if it becomes soaking wet.
Occasionally, fluid will build up in the pleural vent. It is important that you contact the lung clinic if this happens, as it may stop the pleural vent from working properly. A doctor can remove the fluid from a port underneath the drain, using a syringe.
Follow Up
We will follow up your progress in the lung clinic, usually the day after the pleural vent has been inserted. A doctor will review you and will arrange an X-ray of your chest.
The blue indicator diaphragm on top of the pleural vent usually stays fixed in the down position when the air has all gone and the pneumothorax has resolved.
We will remove the pleural vent once the pneumothorax has gone. This simply involves removing the sticky dressing and pulling the device away.
Contact numbers
If you need any further advice or have any problems, please contact the appropriate number below:
Lung Health
Monday – Friday
9.00 am – 5.00 pm
Telephone: 01642 624270
Department of Respiratory Medicine
Monday – Friday
9.00 am – 5.00 pm
Telephone: 01642 624936
Out of Hours – Emergency Department
24 hours a day, 7 days a week
Telephone: 01642 382899
Comments, concerns, compliments or complaints
Patient Experience Team (PET)
We are continually trying to improve the services we provide. We want to know what we’re doing well or if there’s anything which we can improve, that’s why the Patient Experience Team (PET) is here to help. Our Patient Experience Team is here to try to resolve your concerns as quickly as possible. The office is based on the ground floor at the University Hospital of North Tees if you wish to discuss concerns in person. If you would like to contact or request a copy of our PET leaflet, please contact:
Telephone: 01642 624719
Freephone: 0800 092 0084
Opening hours: Monday to Friday, 9:30am to 4:00pm
Email: [email protected]
Out of hours
Out of hours if you wish to speak to a senior member of Trust staff, please contact the hospital switchboard who will bleep the appropriate person.
Telephone: 01642 617617
Data protection and use of patient information
The Trust has developed Data Protection policies in accordance with Data Protection Legislation (UK General Data Protection Regulations and Data Protection Act 2018) and the Freedom of Information Act 2000. All of our staff respect these policies and confidentiality is adhered to at all times. If you require further information on how we process your information please see our Privacy Notices.
Telephone: 01642 383551
Email: [email protected]
Privacy NoticesLeaflet feedback
This leaflet has been produced in partnership with patients and carers. All patient leaflets are regularly reviewed, and any suggestions you have as to how it may be improved are extremely valuable. Please write to the Clinical Governance team, North Tees and Hartlepool NHS Foundation Trust, University Hospital of North Tees, TS19 8PE or:
Email: [email protected]
Leaflet Reference: PIL1238
Date for Review: 16/09/2023
